Mission to care
Medical students get clinical experience at home and abroad
By Laurie B. Davis
Dr. John Wells (Med ’08) remembers the first time he heard the sound of a heart murmur, and that was during his medical program at The University of Toledo. “You listen to so many heart sounds that when you hear that first murmur, you think, I don’t know why this is different, but I know it’s not normal.” His exam of the child with the abnormal heartbeat took place when Wells was a first-year medical student — a clinical experience he had while in Honduras on a global medical mission with Dr. Richard Paat (Med ’86).In February 2018, the two physicians will return to Honduras with another group of medical students who are part of the Students for Medical Missions Program in UT’s College of Medicine and Life Sciences. Another dozen or more alumni who have experienced missions with Paat also will accompany them.
Paat started the global medical missions program at the University in 1998. He had been going on missions to the Philippines since 1994 as a way to give back to people who shared his Philippine roots. Both of Paat’s parents are from the Philippines, and his father also is a doctor. At the end of his first mission there, Paat decided to connect with his own contacts in the country and work with a group of expatriate Filipinos in Toledo to strengthen the missions. “It wasn’t the best planned mission, and at the end of that one, I said, ‘we can do this better.’”
In 1996, he began working with the medical school at the University of Santo Tomas, where his father had graduated from in 1955. “They’ve had a mission program in existence for about 55 years now. So, they knew how to do this the right way.”
They transform schools into hospitals and perform 200 major and 200 minor surgeries. “We see 2,000 patients in the field. Our dentist will do 1,000 tooth extractions. We have an eye team with us who will do 40 to 50 cataract surgeries.” They also conduct other surgeries such as those on the thyroid, and for cleft lips and cleft palates, gall bladders and hysterectomies. “That’s how I got my first taste of how to run a mission and have an impact,” he says.He continued to visit the Philippines every other year. During one of those trips, a Filipino medical student who was at UT joined Paat on a mission. “That’s when we said it would be great to have a mission program in existence for students in order for them to have a service learning opportunity to gain mission experiences, serve the underserved, go to different countries under guidance,” says Paat. “They would learn how to practice medicine without MRIs, CAT scans and be serving people who are really needy.”
That notion was furthered when two PhD/MD students, Scott McLean (Med ’99) and Todd Brickman (Med ’02), had a hallway conversation. McLean expressed to Brickman how great his experience had been on a trip he made to Peru and that other students should have similar opportunities. “They formed an organization and asked me to be their faculty advisor,” says Paat. “They had their first meeting and 100 students showed up. When Hurricane Mitch hit Honduras, the City of Toledo asked me to take a medical team in to assist, and I said I would if I could bring the medical students.”

Paat says someone on the team also will serve as a translator. Wells fell into that role on his first student mission to Honduras. He had lived in Argentina for a time, and after marrying his wife, Emilee, they both worked in an orphanage in Bolivia. When he began medical school at UT, he learned about a medical mission trip with Paat. “I absolutely wanted to go. I speak fluent Spanish and love Latino culture so the opportunity to combine that with medicine was amazing. That first year, I did a lot of translating for the group.” Wells and another student were selected from among 30 applicants. Today, 30 or more students have the opportunity to travel as part of the team.
Disaster missions
UT students first began participating in medical missions in 1998, when they traveled to aid the survivors of Hurricane Mitch in Honduras. The storm was one of the deadliest in Central America’s history, killing 11,000 people, many dying in floods and mudslides from massive rainfall that wiped out their villages. Mitch, Katrina, Matthew, Harvey, Yolanda and Maria are just some of the storms that have devastated areas where Paat has traveled to in the wake of their destruction. Countries in which medical care is among the lacking services, infrastructure, and even basic needs of food, clean water and sanitation, are on a list of repeat missions.“I brought in six students to Honduras in 1998. We were there in November after Hurricane Mitch on Oct. 22. Besides our routine mission to the Philippines, we made a commitment to keep going there,” says Paat. “The following year, we started bringing teams into Guatemala through our St. John’s Jesuit organization; that’s where I graduated from high school in Toledo. Then we started bringing teams into Tanzania through the Toledo Sister City organization. After the Haiti earthquake, we started bringing teams into Haiti.”
Since his first mission to Mindanao, Philippines in 1994, Paat has traveled across the globe for 75 missions. He returned to Yabucoa, Puerto Rico, during the 2017 Thanksgiving holiday to help students from the San Juan Bautista School of Medicine build their own in-country mission program. Yabucoa was one of the first towns hit by Hurricane Maria.
Every mission brings with it challenges, especially if it’s a disaster mission, says Paat. Getting into a country or a U.S. state to temporarily practice medicine there requires the assistance of his liaisons on the ground and the necessary licensing. He reached out to one contact after Hurricane Maria and asked: “Can you get me a letter of invitation from the mayor,” to obtain clearance to go into Yabucoa.
Paat has built over the years relationships with people and organizations that do mission and relief work. As a graduate of St. John’s Jesuit High School in Toledo, Paat has maintained a connection to the school and its charitable work. He has relied on hospitals, churches, universities and humanitarian organizations, such as Catholic Charities or the Salvation Army to host his teams when they’re in the field or to aid their entry into a country. “If the need is there and I have potential contacts there,” says Paat, he’ll find a way to get his team in.
“What we try not to do is get bogged down in red tape, especially in a disaster. Working with the churches is always a quick way, an efficient way because we’re all trying to serve the common good.”
Juanita, dirty water and miles to walk

During that trip, Wells met Juanita. He explains that wheelchairs — always used and donated — are both sparse and coveted in the mission clinics, and a young, determined boy had spotted one. “My sister really needs that wheelchair,” he told Wells. “She hasn’t walked in 30 years and she’s stuck at home in bed.
“He was pretty persistent,” says Wells. He told the boy it would require a house call to visit his sister and check out her condition and physical needs before they could give him the chair. When the boy took Wells to his grandparents’ home, where he and his sister lived, Wells met Juanita. “The first thing I noticed was her huge smile. Her legs are all shriveled and her arms are deformed.” As a childhood victim of polio, Juanita had truly been bed-ridden for 30 years. “I saw a stick with a little mirror attached to the end and asked her, ‘what’s with the mirror’? She can look through it to see behind her through the window on the porch. That’s how she gets to look outside.”
Juanita got her first ride outdoors. “They were so excited for her to be able to get out of the house and go on walks. Something as simple as this; it wasn’t even a fancy or nice wheelchair, but they were just so excited and grateful. When we were leaving, I hopped in the back of the truck, and I looked in her window and saw her little mirror. She was looking at us, and I waved, and she waved her mirror.”
Wells says his biggest challenge on the missions is not being able to do more for patients. Some of the people he meets struggle with physical deformities from earlier injuries that now can only be treated with ibuprofen to ease the pain. “It feels like the help that I have to give is kind of puny, that it’s not adequate, but it’s all I have.”
But his role in coordinating arrangements to bring in clean water filters for families and schools could help stop the spread of intestinal parasites that cause debilitating diarrhea or worse. “There was a pathologist at The University of Toledo named Jim Hampton,” says Wells, “and we found a microscope that someone was willing to donate. We took him and the microscope. At that point, we knew intestinal parasites were a real problem, and we deworm everybody. He took a water sample from every drinking water source and would look at it. I still remember his quote: ‘Man, I don’t know what all this stuff is, but there’s a lot of it and it wiggles.’
“Sawyer makes the filter we’re using now,” says Wells. “They have a big humanitarian branch and they gave us filters at a fraction of the usual cost. You just have to back flush them, and they’re nearly impossible to contaminate. We educate the people on how to use them and clean them. You think about all the vaccines there are, but clean water and sanitation is probably the biggest thing.”
One Sawyer filter can provide 100,000 gallons of clean water, says Paat. “You give them clean water and you give them clean health.”
In Honduras, there’s no electricity or running water, and transportation, for the most part, is on foot. “They start walking before the sun comes up, moms with all the kids, and they walk for miles and miles and hours just to come see us, and they wait in line for hours before they get to triage, and then they wait in line for another hour or two just to get into the clinic,” says Wells. “And they still have a big, bright smile and are happy and grateful. They’re living in staggering poverty but they’re happy. That’s something that has been a lesson to me.”
How to MacGyver in the field
Paat has adapted to diverse circumstances while caring for many people living through tough situations, including day-to-day poverty or hurricanes. “When you’re on the ground during the mission, it’s what do I have and what is the best way I can take care of this patient in this scenario? Sometimes you have to come up with things. We call it ‘MacGyvering.’“There was a little kid in Honduras who had a tracheostomy, and the mom couldn’t afford a suction machine, so the mucus kept plugging, and the kid would end up in the hospital all the time with pneumonia. So, she came and saw us in the clinic. And we said, well, we don’t have a machine, but we had this wound drainage reservoir that if you pushed it down it produced a vacuum, and we found a little suction thing and we hooked them up together. We taught the mother how to suction her child. And that’s MacGyvering.”
By practice, internists do not deliver babies, but Paat delivered one in Tanzania. “They named the baby after me,” he says. As followers of the Hippocratic Oath of “first do no harm,” they do try to find a way to treat the patient with the resources they have. Seventy-five missions and 112,000 patients later, Paat says, “I’ve seen a lot things. My knowledge base has improved. You have to know how to deliver babies, do an amputation. Before the Haiti earthquake, I didn’t know how to do an amputation, so I watched a YouTube video on how to do an amputation, and I said, ‘OK, I guess I could do that if I had to.’ Thank goodness, we had orthopedic surgeons with us.”
A sustainable network of care
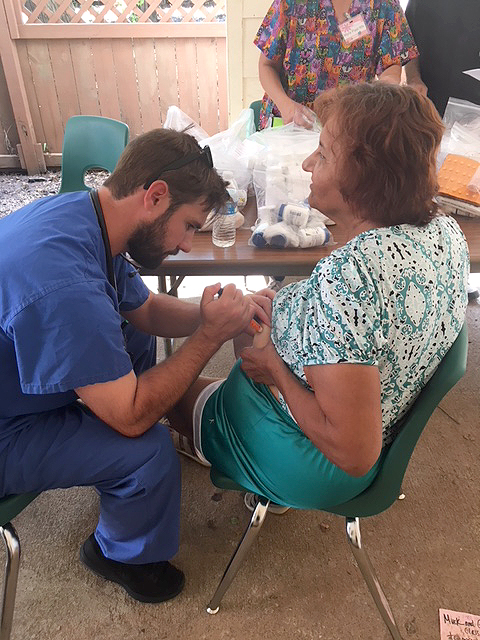
Texas city.
The medical students train the villagers who will earn a certificate for completing the course. “Over the course of a week they’re with us, we train them to deliver babies, how to use a stethoscope, a blood pressure cuff, how to treat diarrhea, malnutrition, how to diagnose basic things. We train them how to ask the right questions,” says Paat.
“We leave them with a cache of medicines that they know how to use; things like Tylenol, Motrin, some antibiotics, creams. We leave them with a blood pressure cuff, stethoscope and a training certificate that they’re really proud of, and with wound care materials and their book.”
As a health promoter with a certificate and a guidebook their neighbors know they have rudimentary medical training and can rely on them for care. Sometimes the nearest hospital can be 40 or more miles away from a village, and a patient would have to walk there. Paat and his teams of students have trained people in 60 different villages around the world, including in Haiti, Tanzania, Guatemala and Honduras.
It seems that with every new contact Paat makes, the network of medical missions expands, giving more students clinical experiences and more patients access to medical care. Paat has helped Marshall University in West Virginia establish a medical mission and is working now with students in Puerto Rico to create their own to visit people in the mountains.
“Though initially a way to give back to my parents’ home country, the medical missions program has kind of morphed into a way of teaching students and providing a service learning opportunity, to bringing in clean water, to a training program; we do it all.”










